Erkeklerin Görünmez Sorunu: HPV ve Siğil Tedavisinde “Nüks” Bilmecesi, Doç. Dr. Tevfik Ziypak, Üroloji Uzmanı’nın klinik deneyimleri ve bilimsel veriler ışığında değerlendirdiği önemli bir sağlık başlığı olarak öne çıkıyor.
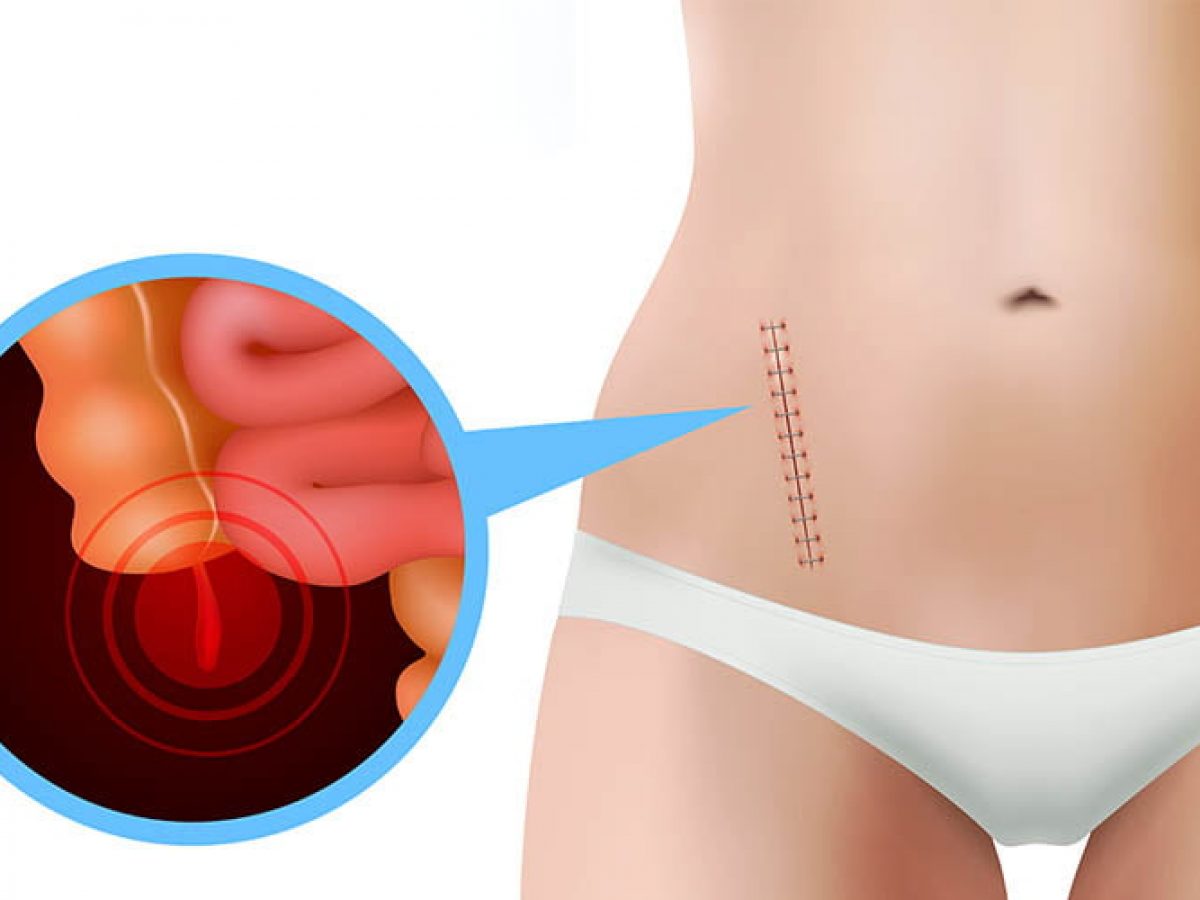
Toplumda genellikle kadın sağlığı ve rahim ağzı kanseri ile ilişkilendirilen HPV (İnsan Papilloma Virüsü), aslında erkek sağlığını da yakından ilgilendiren, ancak çoğu zaman ihmal edilen bir tabu. Bir üroloji uzmanı olarak poliklinikte en sık karşılaştığım vakaların başında gelen genital siğiller (kondilomlar), sadece fiziksel bir sorun değil, hastanın psikolojisini ve cinsel yaşamını da derinden etkileyen "bitmek bilmeyen bir döngü" halini alabiliyor.
Tedavide Neden Başarısız Olunuyor?
Hastalardan en çok duyduğumuz şikayet: "Hocam, siğilleri yaktırdım ama 2 ay sonra tekrar çıktı." Bu durumun temel sebebi, tedavinin sadece "görünen" siğile odaklanmasıdır. HPV bir cilt enfeksiyonudur ve virüs, siğilin çevresindeki görünüşte sağlıklı olan deride de yaşamaya devam eder. Eğer tedavi planı sadece o anki lezyonu yok etmek üzerine kurulursa, nüks kaçınılmazdır. Bugün modern ürolojide başarı; siğili yakmak değil, nüksü önleyecek bir bağışıklık stratejisi geliştirmektir.
Kriyoterapi ve Elektrokoter: Klasik Ama Etkili
Doğru ellerde uygulanan Kriyoterapi (dondurma) ve Elektrokoter (yakma) yöntemleri hala altın standarttır. Buradaki kritik nokta, cerrahın deneyimidir. Derinliği iyi ayarlanmamış bir yakma işlemi hem ciddi iz (skar) bırakabilir hem de virüslü dokunun tam temizlenememesine neden olabilir. Üroloji uzmanının anatomik bilgisi, özellikle hassas olan penis ve idrar kanalı çevresindeki lezyonlarda doku bütünlüğünü korumak için hayati önem taşır.
Bağışıklık Sistemi: En Güçlü Silahımız
2026 yılına geldiğimizde, HPV tedavisinde sadece "yok edici" değil, "destekleyici" yaklaşımlar ön plana çıkıyor. Tedavi sonrası bölgeye uygulanan bağışıklık düzenleyici kremler ve hastanın yaşam tarzı değişiklikleri virüsün vücuttan temizlenme hızını doğrudan etkiliyor.
Hastalarımızın En Çok Merak Ettiği 4 Kritik Soru
1. Prezervatif kullanımı HPV’den tamamen korur mu? Maalesef hayır. Prezervatif risk oranını düşürse de, HPV cilt temasıyla bulaşan bir virüstür. Prezervatifin kapatmadığı kasık ve testis bölgelerindeki temas, virüsün bulaşması için yeterli olabilir.
2. Siğil yoksa bulaştırıcılık biter mi? Hayır. Gözle görülür bir siğil olmasa bile virüs deride uykuda (latent fazda) kalabilir ve bulaşmaya devam edebilir. Bu nedenle "siğilim geçti, artık güvendeyim" demek için erken olabilir.
3. Ortak kullanım alanlarından (havuz, tuvalet, havlu) bulaşır mı? HPV’nin bu tür yüzeylerden bulaşma ihtimali teorik olarak çok düşüktür. Bulaşın ana yolu %99 oranında doğrudan cilt temasıdır.
4. Aşı konusu: "Geç Kaldım mı?" Dünya Sağlık Örgütü’nün (WHO) güncel tavsiyeleri, HPV aşısının sadece çocuklar için değil, aktif siğil tedavisi gören yetişkin erkekler için de bir "koruma kalkanı" olabileceğini gösteriyor. Aşı mevcut siğili iyileştirmese de, vücudun diğer HPV tiplerine karşı direncini artırıyor.
Utanmak Tedaviyi Geciktirir
Erkek hastaların en büyük hatası, utandıkları için süreci kendi başlarına çözmeye çalışmaları veya "bitkisel" yöntemlerle vakit kaybetmeleridir. HPV, doğru yönetildiğinde kontrol altına alınabilen bir süreçtir. Önemli olan, sorunu bir uzmana danışmak ve "tek seferlik bir işlem" yerine "sürece yayılmış bir takip" planına sadık kalmaktır.
Unutmayın; siğiller geçer, önemli olan vücudun bu savaşı kazanmasını sağlamaktır.
Sağlıklı günler dileriz.